It’s Time to Stop Prescribing Points

By Dr. Bruce Park, DACM
WHAT YOU NEED TO KNOW
- The term prescription smuggles in a pharmaceutical logic: find the right agent, deliver it and expect a result. Drug > Administration > Effect. When translated into needling, this becomes: Point > Insertion > Effect.
- A generation of graduates can recite point combinations with poetic precision but lack the tactile intelligence to respond when a patient’s body contradicts the textbook.
- If expertise is defined as memorizing lists, we can be replaced by an algorithm. But if expertise is defined as sensing, deciding, modulating, and confirming, the practitioner becomes irreplaceable.
In a quiet corner of a busy teaching clinic, a student stands over a patient, needle poised. They have a “perfect” prescription: a textbook combination of points harvested from a lecture slide on chronic lower back pain. But as the needle meets the skin, the student hesitates. The tissue is dense, resisting entry. The patient’s breath is shallow. The student looks at the chart, then at the point, waiting for a result that hasn’t arrived. They know the map perfectly, but they are lost in the landscape.
The Problem With Our Vocabulary
This hesitation is the symptom of a quiet habit that has taken hold of our profession. In our classrooms, treatment rooms and journals, we routinely say we “prescribe” points. It sounds efficient. It echoes the authority of biomedical culture and fits neatly into the insurance field. But vocabulary is never neutral; repeated long enough, it dictates behavior.
The term prescription smuggles in a pharmaceutical logic: find the right agent, deliver it and expect a result. Drug > Administration > Effect. When translated into needling, this becomes: Point > Insertion > Effect. The symmetry is elegant, but it is fundamentally false.
The Huangdi Neijing does not describe a world of automatic reactions.1 It describes a world of regulation, timing and response. It places the burden of efficacy on the practitioner’s capacity to recognize change and guide it. Without the engagement of qi, there is a position but no therapy. When we “prescribe,” the practitioner risks becoming a mere delivery mechanism. To reclaim our identity, we must shift toward a more faithful phrase: point selection strategy.
The Hidden Curriculum
Every training program runs two syllabi. One is printed in the handbook; the other is whispered in everyday speech. When learners constantly hear about “prescriptions,” they begin to believe that effects are inherent in the points themselves – that technique is decorative, and deqi is optional.
The result is a generation of graduates who can recite point combinations with poetic precision but lack the tactile intelligence to respond when a patient’s body contradicts the textbook. By shifting our language to strategy, the paradigm transforms. Points become portals rather than pills, and the practitioner becomes the instrument rather than the administrator. Competence moves from rote recall toward sensory perception.
A Point Is Not a Pill
A medication is designed for chemical stability; a needle is a tool of modulation. An acupuncture outcome varies wildly based on angle, depth, pacing, and the patient’s readiness. As Hugh MacPherson noted, tightly scripted protocols often fail to resemble the clinical reality where adaptation defines effectiveness.2
If the effect depends on the feedback loop between hand and tissue, the word prescription collapses a living exchange into a static list. Our resemblance to biomedicine might increase, but our clinical accuracy decreases.
Consider a chef. A recipe describes potential, but dinner only happens when the cook senses the heat and aroma and makes a real-time correction. Two people can follow the same instructions; one produces nourishment, the other produces mere compliance. The difference is judgment.
What “Strategy” Looks Like in Practice
A strategy-based approach recognizes that selection only prepares the field. The true arc of treatment looks like this:
- Diagnosis: Identifying the pattern
- Strategic Entry: Choosing the points
- Method and Modulation: The physical craft of needling
- Qi Movement (qizhi): The initiation of change
- Confirmation (deqi): The perception of engagement
- Regulation: Stabilizing the system
This sequence makes clinical reasoning visible. A chart note that simply lists “LI 4, LV 3” is just geography. A strategy-based note – “Distal-local regulation initiated; bilateral deqi obtained; myofascial guarding reduced” – is evidence of a thinking clinician.
The Stakes of Our Language
If expertise is defined as memorizing lists, we can be replaced by an algorithm. But if expertise is defined as sensing, deciding, modulating, and confirming, the practitioner becomes irreplaceable.
Invisible labor – the subtle adjustments we make at the needle head – is often undervalued labor. Precision in our language protects the value of what we actually do. It reminds the world that acupuncture is not just something we give; it is a craft we perform.
Where Change Begins
We do not need a reform committee to fix this. We simply need to ask better questions. In our clinics, let us stop asking “What is the point for X?” Instead, let us ask: “What is my intention? What movement is required? Where is access available right now?”
When our speech evolves, our training follows. When our training follows, our care deepens. It is time to stop prescribing points and start teaching a strategy. Because points open doors, but they do not walk through them.
References
- Unschuld PU. Nan Jing: The Classic of Difficult Issues, 2nd Edition. University of California Press, 2016.
- MacPherson H, Hammerschlag R. Acupuncture and the emerging evidence base: contrived controversy and rational debate. J Acupunct Meridian Stud, 2012 Aug;5(4):141-7.
April 2026
https://acupuncturetoday.com/article/39999-its-time-to-stop-prescribing-points
Qizhi to Deqi: The Living Sequence That Animates Acupuncture
By Dr. Bruce Park, DACM
WHAT YOU NEED TO KNOW
- All too often, acupuncture is reduced to protocols, checklist, and point prescriptions. But the deeper work begins when we shift our focus – from treating symptoms to engaging systems; from targeting points to connecting with the person.
- Qizhi flows; deqi is connection. One initiates the current; the other affirms the therapeutic resonance.
- Before your next needle insertion, pause and ask: Have I sensed the movement of qi? Has the patient affirmed its arrival? Has resonance replaced resistance? These are more than procedural steps – they are gateways into the therapeutic relationship.
In the art of acupuncture, two concepts – qizhi (qi arrival) and deqi (obtaining qi) – form the clinical foundation of effective needling. Though often used interchangeably, they describe distinct and sequential phases of therapeutic engagement. To truly feel and guide qi, a practitioner must learn to embody this classical sequence, recognizing qizhi as the current that is initiated and deqi as the resonance that is confirmed.
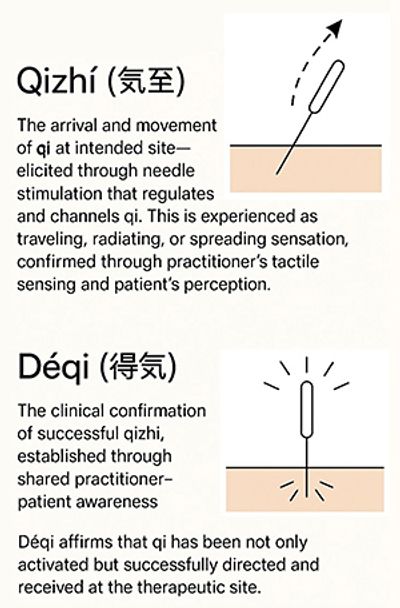
Qizhi: The Arrival and Movement of Qi
First, there is qizhi. I define this as a dynamic, functional process – the arrival and directional movement of qi at a targeted site. Through skillful, guided stimulation, qi is not merely activated; it is conducted with intention toward its therapeutic endpoint. This is the moment your treatment becomes kinetic; a tangible flow you can perceive through a confluence of patient sensation and your own tactile feedback.
- Your Patient's Experience: They may report a traveling, radiating or wave-like sensation; a feeling of warmth or pressure moving along a defined pathway.
- Your Tactile Observation: You will feel an elastic tension under the needle, a shifting tissue tone, or the subtle “pull” or “grasp” that signals movement.
“When the qi arrives, the effect becomes evident. Its impact is as certain as the wind that scatters clouds, as clear as the blue sky that follows.” — Huangdi Neijing Lingshu, Chapter 3
Qizhi is the energetic current – the vital signal that the therapeutic process has begun.
Deqi: The Confirmation of Shared Awareness
Following qizhi, you seek deqi. I define this as the clinical confirmation that qi has not only arrived, but also has been successfully received, anchored, and acknowledged. More than just a sensation, deqi is a relational event – a mutual awareness between practitioner and patient that a therapeutic threshold has been crossed.
This shared moment of recognition is often marked by unmistakable cues:
- From Your Patient: A spontaneous deep sigh, an emotional release, a visible softening of their facial expression, or a felt sense of resolution and inner stillness.
- From Your Hands: A palpable softening of the local tissues, a subtle vibration that replaces tension, or a clear harmonization of the patient's breath and radial pulse.
- Deqi marks the moment the body affirms the connection: “Yes, the qi is here, and I am responding.”
Case Vignette
A 42-year-old patient presents with chronic neck and shoulder tension. After the practitioner needles SI 15 and GB 21 with breath-guided insertion, the patient reports a wave of warmth spreading down the arm – a classic presentation of qizhi. Moments later, you observe her exhale deeply and smile without prompting. . Simultaneously, you sense a distinct softening of the trapezius muscle and feel a smoother, more harmonious quality in her radial pulse. With these cues, you have confirmed deqi.
The Five Gates Model
This clinical sequence finds its structured home within the Five Gates needling model I teach:
- Perceiving qi (chaqi): Your initial sensory awareness and observation
- Guiding qi (daoqi): Your intentional direction of qi with breath and touch
- Moving qi (xingqi): Your responsive stimulation to initiate flow
- Obtaining qi (deqi ): Your confirmation of arrival and resonance
- Stabilizing qi (shouqi): Your final anchoring and integration of the effect
At gate four, you consciously shift from doing to listening. It is here that your technique becomes a relationship. Your needle, no longer a mechanical tool, becomes an instrument of awareness, shaped by your intention and spirit.
Bridging Ancient Wisdom and Modern Science
This clinical sequence of flow and confirmation is not merely a poetic construct; it is directly reflected in distinct physiological events now being mapped by modern science. While classical texts like the Huangdi Neijing Lingshu established the importance of these phenomena,1 contemporary research provides a modern blueprint for the biological processes that underpin them.
- The Neurosensory Current of Qizhi: The traveling and radiating sensations of qizhi correlate directly with the activation of specific Aδ and C-nerve fibers. Psychophysical studies confirm that this subjective experience generates a complex signal engaging both spinal and central pathways, providing a neurological explanation for the "flow" felt by the patient.2
- The Biomechanics of Needle Grasp (Qizhi): The practitioner's tactile sensation of "needle grasp" has a clear biomechanical origin. Research shows that rotating a needle causes subcutaneous connective tissue and fascial planes to wind around it. This mechanical coupling initiates a cellular signaling cascade known as mechanotransduction, which can propagate along meridians and explains the practitioner's tangible perception of qizhi.3
- The Systemic Confirmation of Deqi: The state of deqi – marked by a deep sigh, emotional release, and a sense of resolution – is mirrored by profound changes in the central nervous system. Functional MRI studies reveal that acupuncture modulates the limbic system, the brain's hub for emotion and memory. This provides a clear neurological basis for the autonomic shift and inner stillness that confirm the therapeutic connection has been made.4
From Needle Insertion to Therapeutic Resonance
Too often, acupuncture is reduced to protocols and point prescriptions. The deeper work, however, begins when we shift our focus from treating symptoms to engaging systems; from targeting points to connecting with the person.
- Qizhi flows.
- Deqi confirms.
- Together, they initiate transformation.
Before your next needle insertion, pause and ask: Have I truly sensed the movement of qi? Has the patient affirmed its arrival, verbally or non-verbally? Has resonance replaced resistance in the tissue?
These are not procedural checkboxes; they are gateways into the therapeutic dialogue. When you approach acupuncture as a conversation, rather than a directive, your technique is elevated by mindfulness, and healing unfolds not just from a needle, but through connection.
References
- Unschuld PU, Tessenow H. (Trans.) Huang Di Nei Jing Ling Shu: The Ancient Classic on Needle Therapy. University of California Press, 2011.
- Kong J, Gollub RL, Fufa DT, et al. Brain activity associated with the acupuncture sensation of déqì: A psychophysical study. Human Brain Mapping, 2005;24(3):189-199.
- Langevin HM, Churchill DL, Wu J, et al. Subcutaneous tissue fibroblast cytoskeletal remodeling induced by acupuncture: evidence for a mechanotransduction-based mechanism. J Cell Physiol, 2002;191(3):321-327.
- Hui KKS, Liu J, Makris N, et al. Acupuncture modulates the limbic system and subcortical gray structures of the human brain: evidence from fMRI studies. Human Brain Mapping, 2000;9(1):13-25.
August 2025
Why Acupuncture Is Becoming the Smart Choice for Pain Relief

By Dr. Bruce Park, DACM
More people today are looking for better ways to manage pain—options that don’t depend on endless pills, repeated injections, or risky surgeries. The pattern has become familiar: something hurts, an MRI is ordered, the scan shows “damage,” and surgery quickly enters the conversation.
But many patients pause and ask:
- “Is surgery really the only answer?”
- “Why does the pain keep coming back even after treatment?”
- “Is there a safer, more natural way to heal my body?”
This is exactly where acupuncture shines. It’s becoming the first choice for many patients—especially those who research, ask questions, and want a comprehensive, whole-person approach to healing.
Pain Is About More Than What Shows Up on an MRI
Here’s an important fact: many “abnormal” findings on scans—disc bulges, arthritis, wear-and-tear—are found in people who have no pain at all. These changes are simply part of aging, like wrinkles or gray hair.
Meanwhile, real pain is influenced by everyday factors such as:
- tight or weak muscles
- reduced circulation
- stress and tension
- poor sleep
- old injuries
- movement habits and posture
These are precisely the areas where acupuncture makes a difference. It addresses the functional, day-to-day contributors to pain—the things surgery cannot fix.
A Natural Way to Reset Your Body
People are often surprised by how quickly their bodies respond to acupuncture. A few thin, gentle needles can:
- relax tight muscles
- improve blood flow
- calm the nervous system
- reduce inflammation
- soften long-held tension
- promote deep relaxation
It isn’t magic—it’s your body waking up its own healing system. Acupuncture gives your body the space to reset, recover, and restore balance without adding more stress.
A Safer Step Before Considering Surgery
Of course, surgery has its place. But for many common pain problems—back pain, neck tension, shoulder issues, knee aches—research shows that surgery often doesn’t outperform good conservative care.
And surgery comes with real risks:
- long recovery times
- scar tissue
- possible nerve irritation
- unpredictable results
Acupuncture gives patients a safe, low-risk option to try first. Many people who come to my clinic expecting that surgery is their only choice end up avoiding it altogether because their pain improves significantly with acupuncture.
Why More People Are Turning to Acupuncture
People today want treatments that are:
- simple and accessible
- natural and low-risk
- focused on the whole person
- supportive of both body and mind
- effective without heavy medications
Acupuncture meets all of these needs. It works with the body instead of overpowering it. Patients often feel not only less pain, but also more centered, calmer, and more energized.
A More Mindful Way to Heal
In my practice, I use Mindful Acupuncture Practice (MAP), a system that blends classical acupuncture, modern anatomical understanding, and mindful awareness. This approach helps patients not only reduce pain but also understand how their body moves, breathes, and responds to stress.
Patients often share:
- “Acupuncture gives me hope.”
- “My whole system relaxes.”
- “It feels like my body can finally heal.”
This is the heart of acupuncture—healing that begins from the inside out.
You Deserve More Than Pain Pills and Scary Options
Pain can feel overwhelming. It can make you feel stuck, frustrated, or unsure of what to do next. But you have more options than you think. Acupuncture is one of the safest, most effective, and most natural treatments available today.
If you’re struggling with back pain, knee pain, neck tension, stress-related tightness, headaches, or chronic discomfort, acupuncture is a gentle and intelligent place to begin. It helps your body remember how to heal—and it does so without the risks of surgery or long-term medication use.
Your body wants to feel better. Acupuncture gives it the chance.
MINDFUL ACUPUNCTURE PRACTICE (MAP)

What is Mindful Acupuncture Practice?
Mindful Acupuncture Practice (MAP) is a comprehensive clinical model that unites classical acupuncture principles, modern biomedical science, and the discipline of mindful presence into a single, coherent approach. At its core, MAP emphasizes that the effectiveness of treatment arises not only from technical skill but from the practitioner’s inner cultivation. Presence, compassion, and precision are regarded as decisive factors in shaping therapeutic outcomes, transforming the act of needling into a dialogue between practitioner and patient. By weaving together traditional channel theory, evidence from contemporary physiology, and the art of mindful awareness, MAP offers a framework that honors both the science and spirit of healing.
Principles and Strategies
These sources provide an extensive overview of a clinical model called Mindful Acupuncture Practice (MAP), which integrates traditional East Asian medicine, modern biomedical science, and mindful presence. The text outlines the philosophical foundation, emphasizing the practitioner’s non-digitizable skills, and details the Phased Intervention Priority System (PIPS) for strategic treatment planning and the Interactive Needling Practice (INP) for precise, responsive technique. Chapters and appendix excerpts cover specific diagnostic methods like layered palpation and pulse reading, therapeutic protocols such as the Five-Pinpoint Integrated Needling System (5PINS) and Cranial Nerve Acupuncture, and case studies illustrating the application of these integrated strategies. The material also includes educational frameworks for teaching MAP, stressing the importance of mindful communication and professional ethics.
The Thinking Hand
The cultivated hand of the practitioner—alive, perceptive, and responsive. It embodies perception, knowledge, and spirit in action, transforming acupuncture from a mechanical technique into a therapeutic art. As a living instrument that bridges theory with embodied reality, the thinking hand is regarded as acupuncture’s most human technology. Watch an audio clip.
Redefining Acupuncture Through Precision and Mindfulness

What is Mindful Acupuncture Practice?
The Mindful Acupuncture Practice (MAP) represents a transformative evolution in acupuncture education and clinical methodology. It introduces a system that transcends both conventional, mechanical approaches and traditional methods reliant on rote learning or fixed protocols. At its core, MAP integrates classical wisdom, modern scientific insight, and contemplative awareness—redefining the practitioner’s internal state (Shen) as the central therapeutic instrument.
1. The Practitioner's Presence as the Primary Therapeutic Instrument
MAP's most fundamental concept is that the efficacy of treatment is inseparable from the cultivated presence, mindfulness, and awareness of the practitioner.
- Wholehearted Care (Jingcheng): This is the core ethical and clinical philosophy, representing the courageous synthesis of refined technical mastery (Jing) with sincere compassion (Cheng). This ideal elevates acupuncture from a technique to an art of healing.
- Shen as Mirror and Tool: The book emphasizes that true healing is guided by the cultivated Shen (spirit/mind/innate intelligence) of the practitioner and must begin with perceiving the Shen of the patient.
- Contemplative Integration: MAP draws on decades of contemplative awareness, including the author's time as a Buddhist monk, teaching that breath cultivated in stillness anchors palpation and mindfulness sharpens perception. This process of self-cultivation distinguishes mastery from mere technical proficiency.
- The "Thinking Hand": The practitioner cultivates a "thinking hand" that is alive, perceptive, and responsive, serving as the living interface where knowledge, perception, and intention converge. This is presented as humanity’s "most human technology," which cannot be replicated by AI.
2. Systematic Methodologies for Strategic Treatment Design
MAP provides three structured systems—PIPS, INP, and 5PINS—that replace formulaic or "cookbook" approaches.
A. Interactive Needling Practice (INP)
INP is the core therapeutic method that reframes needling as a co-regulated, somatic dialogue rather than a mechanical act.
- The Five Gates (PIMCH): INP organizes the entire needling sequence into five structured yet fluid stages: Perceiving Qi (Chaqi), Introducing Qi (Daoqi), Mobilizing Qi (Yunqi), Confirming Qi (Deqi), and Holding Qi (Shouqi). This provides a structured, teachable way to engage the body’s innate intelligence.
- Confirming Qi (Deqi) through Latency: The system distinguishes between Qizhi (the local arrival of Qi, the "signal sent") and Deqi (the systemic resonance or "echo returned"). The latency window—the intentional pause between these two events—is treated as a diagnostically meaningful period of "sacred stillness" where healing matures.
- Microexpression Sensitivity: INP integrates the reading of subtle, involuntary patient cues (microexpressions in the face, breath, and posture) to guide treatment, elevating the practice from a purely tactile dialogue to a whole-body conversation.
B. Phased Intervention Priority System (PIPS)
PIPS is a strategic clinical reasoning framework designed to construct elegant treatment plans by addressing the root before the branch. It acts as a "top-down" approach, focusing on systemic coherence.
- Five Progressive Phases: Treatment is hierarchically organized across five layers: Foundational Regulation (stabilizing the constitutional blueprint), Channel Regulation (restoring primary flow), Organ Regulation (harmonizing Zangfu), Symptomatic Resolution (addressing chief complaint), and Spirit Integration (restoring psycho-emotional harmony).
C. Five-Pinpoint Integrated Needling System (5PINS)
5PINS is a minimalist, precision-based framework that aims for profound results with minimal intervention. It acts as the "bottom-up" engine for resolving structural and functional dysfunction.
- Functional Layered Diagnosis: 5PINS integrates classical theory with neuroanatomy, focusing on five distinct therapeutic functions/layers: Systemic & Autonomic Regulation, Segmental & Channel Harmonization, Symptom Modulation (trigger points), Functional Restoration (motor points), and Central Integration.
- Neuro-Myofascial Integration: The system explicitly incorporates precise targeting of Myofascial Trigger Points (MTPs) and Neuromuscular Motor Points (NMPs) alongside classical Acupuncture Points (ACPs), distinguishing between them by their function (pain generator vs. functional reset). This stems directly from its foundational heritage in Acupuncture Physical Medicine (APM).
3. Innovative Integration Models
The book outlines specialized systems that explicitly bridge classical Chinese medicine with modern biomedical concepts:
- Neuroendocrine Regulation Acupuncture (NERA): This specialized system synthesizes Zangfu theory with modern neuroendocrinology to modulate the major hormonal feedback loops (HPA, HPT, HPG axes). It introduces Neuroendocrine Nodes (NENs)—classical points selected for their documented neurohormonal influence—as a targeted treatment tool.
- Cranial Nerve Acupuncture (CNA): This system systematically maps classical channels and points onto Cranial Nerve Nodes (CNNs) (especially V, VII, and X) to simultaneously treat local facial disorders (like Bell's palsy) and systemic autonomic/neuroendocrine dysregulation.
• • Acupuncture Manual Therapy (AMT): AMT systematizes the integration of hands-on methods (like tuina) with needling, defining a unique sequence based on whether the condition is acute (manual therapy first) or chronic (acupuncture first).
4. Educational and Professional Innovations
The book proposes structural changes for training practitioners to maintain relevance in modern healthcare:
- The Three-Division Model for Education: This is a revolutionary blueprint for mindful pedagogy that trains practitioners to be multilingual in medicine by structuring the curriculum into three integrated domains: Traditional Acupuncture (TA), Modern Acupuncture (MA), and Acupuncture Therapeutics (AT).
- The Five Foundations of Healthy Living (FFHL): This model is a modern clinical application of the classical principle of Yangsheng (nourishing life). It provides a practical, structured framework for patient self-care across five domains (mindful nourishment, restorative sleep, joyful movement, regulatory breathing, and embodied mindfulness) to sustain clinical gains.
Mindful Acupuncture Practice redefines acupuncture as a living, contemplative art grounded in scientific rigor. Its core principle—“the practitioner’s presence precedes the needle”—embodies a shift from mechanical intervention to mindful interaction, from symptomatic relief to systemic harmony, and from technical proficiency to healing intelligence.